We are just weeks shy of the one-year anniversary of the President’s declaration of the COVID-19 National Emergency, and the COVID-19 National and Public Health Emergencies are still in effect. As a result of the long-term impact of the pandemic, many employees faced forfeiting their unused health FSA and dependent care assistance program (DCAP) funds at the end of the 2020 plan year.
As a result, and as we previously reported, a second stimulus relief bill (the Consolidated Appropriated Act, 2021) was signed into law on December 27, 2020, which provided much-needed relief for health FSAs and DCAPs. On February 18, 2021, the IRS released Notice 2021-15, which provides additional guidance related to the relief in the stimulus bill as well as further relief for cafeteria plans and HRAs. The guidance and relief are summarized in more detail below.
IRS Guidance Related to the Second Stimulus Bill (CAA, 2021)
Health FSA and DCAP Carryovers – The stimulus bill authorized employers offering a DCAP or health FSA to allow participants to carry over all unused DCAP and health FSA contributions or benefits remaining at the end of the 2020 plan year to the 2021 plan year. Notice 2021-15 clarifies that:
- Employers may require employees to make an election in the 2021 or 2022 plan year to access the carryover from the previous plan year.
- The carryover relief applies to all health FSAs, including limited purpose health FSAs.
- If an employee uses the mid-year election change relief discussed elsewhere in this alert to prospectively elect to participate in the health FSA mid-year, the employee can access the full amount of their carryover from 2020 retroactive to January 1, 2021.
- Employers can restrict the amount employees can carryover, i.e., they do not have to allow the full unused amount from 2020 or 2021. Employers need to specify the limit to employees in the plan amendment and any communications to employees.
- Employers may allow employees to opt out of the carryover to preserve HSA eligibility.
- The amount carried over may be from multiple plan years, i.e., if an employee has a remaining balance at the end of the 2020 plan year and it is still remaining after the end of the 2021 plan year, it will be accessible during the 2022 plan year (as a carryover) if the employer adopts the carryover relief for the 2021 plan year.
Extended Grace Period – Employers offering a DCAP or health FSA may extend the grace period for using any benefits or contributions remaining at the end of a plan year ending in 2020 or 2021 to 12 months after the end of the applicable plan year. The Notice clarifies that:
- The extended grace period is available for up to 12 months, meaning employers may elect a shorter period of time.
- The relief applies to both general purpose and limited purpose health FSAs.
- For purposes of HSA eligibility, employers can permit employees to opt out of the extended grace period.
Spend Down – Similar to DCAPs, employers offering a health FSA may allow participants who cease participation during the 2020 or 2021 plan year to continue to be reimbursed from any unused benefits through the end of the plan year (and applicable grace period) in which participation ceased. In Notice 2021-15, the IRS clarified the following:
- Employers do not have to allow employees who terminate mid-year to spend down for the remainder of the plan year. Instead, they can adopt a shorter period of time.
- The spend-down can be used for anyone who terminates employment, loses eligibility for the plan due to a reduction in hours, or loses eligibility because they made a new election during calendar year 2020 or 2021.
- Even if the employer adopts the spend-down relief, it must still offer COBRA for individuals with an underspent health FSA account. The COBRA premium established by the employer cannot include the amount carried over or available due to the extended grace period relief.
DCAP Reimbursement for Children Who Turned 13 During the Pandemic – Employers offering DCPAs in plan years with open enrollments that ended on or before January 31, 2020 may choose to reimburse employees for dependent care expenses for children who turned 13 during the pandemic. The relief applies for the subsequent plan year (e.g., calendar year 2021 plans) to the extent the employee has a balance at the end of the 2020 plan year after any relief adopted by the employer. The IRS clarified that:
- The employer may adopt this relief without also adopting the extended grace period or carryover.
Health FSA and DCAP Election Changes – Employers offering a health FSA or DCAP may allow employees to make prospective election changes (subject to annual limitations) to their 2021 contributions without experiencing a change in status event. The IRS clarified the following:
- Employers may allow employees to make the following changes on a prospective basis:
- Make one or more elections; or
- Increase or decrease an existing election
If an employee elects to revoke DCAP or health FSA expenses, the employer may not refund any contributions to employees. The employer may choose to treat the contributions made before the elections are revoked the following ways:
- The contributions may remain available to reimburse medical or dependent care expenses incurred for the rest of the plan year;
- The contributions are only available to reimburse expenses incurred before the revocation takes effect (and not later incurred expenses); or
- The contributions are forfeited.
If the employer takes the second or third approaches listed above, then the health FSA is no longer treated as HSA-disqualifying coverage. Therefore, an impacted employee could begin participating in an HSA as soon as health FSA participation is terminated.
Other FSA Clarifications
The IRS further clarified that employers may adopt an extended grace period or carryover, but not both. Employers can adopt some, all, or none of the FSA relief provided under the stimulus bill. The relief is also available to employers who previously did not offer a carryover or grace period – they can adopt them for the 2020 and 2021 plan years so employees may benefit from the relief.
Further, the employer can adopt relief for some, but not all health FSA or DCAP participants, subject to nondiscrimination rules; however, any amount carried over or the extended grace period will not be taken into account for purposes of nondiscrimination testing.
Additionally, the IRS clarified that, for purposes of the relief, employers may amend the plan to allow employees to make a mid-year election to be covered by a general purpose health FSA for part of the year and a limited purpose health FSA for the remainder of the year. If the employee does so, then any permissible HSA contribution is based on the number of months the employee was covered under the limited purpose health FSA. Further, unused amounts in the limited purpose health FSA can be transferred to the general purpose health FSA or vice versa; however, the general purpose or limited purpose health FSA can only reimburse applicable (based on the type of health FSA), allowable expenses incurred after the change in coverage, respectively. If, under the relief, an employee makes a mid-year election change from an HDHP to a non-HDHP mid-year and elects to participate in a health FSA, then the health FSA must be operated as a limited purpose health FSA for the months the employee was otherwise HSA-eligible, and then may operate as a general purpose health FSA for the remaining months (when the employee was not enrolled in HDHP coverage).
Finally, the IRS clarified that in no instance can an employee receive a refund of any unused FSA contributions in cash or in another form of taxable or non-taxable benefits.
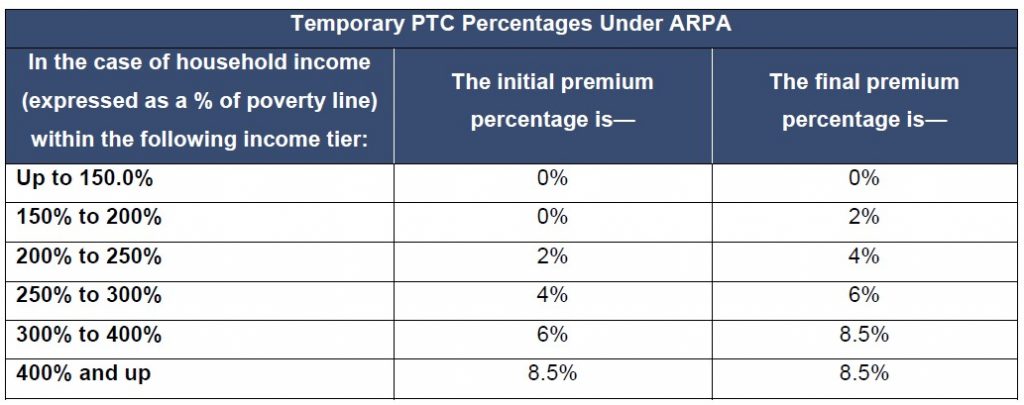
Unfortunately, the IRS failed to clarify with any certainty whether an employee may be taxed on any DCAP reimbursements in excess of $5,000 for the calendar year. While the relief provides that the annual limits under Section 129(a) of the Code apply to amounts contributed to the DCAP for the plan year, not the amounts reimbursed or available for reimbursement, if the employer adopts the extended grace period or carryover, this does not directly answer the question. The guidance does, however, clarify that the W-2, Box 10 amount for the DCAP does not need to be adjusted to take into account the amount available in the extended grace period or carryover. We also note that the American Rescue Plan Act of 2021, a bill to enact President Biden’s COVID-19 relief package, includes a provision that, if passed, would increase the DCAP exclusion from $5,000 to $10,500 (from $2,500 to $5,250 in the case of a separate return filed by a married individual) for 2021.
Additional IRS Relief
Notice 2021-15 also includes additional relief for cafeteria plans and HRAs.
Election Changes for Health Coverage – Similar to the IRS’ initial COVID-19 relief issued last year in Notice 2020-29, Notice 2021-15 allows employers to amend their cafeteria plan to allow employees to make mid-year election changes with respect to employer-sponsored health coverage. Specifically, employers may allow employees to do the following on a prospective basis:
- Make a new election if the employee initially declined coverage;
- Revoke an existing election and make a new election to enroll in different health coverage sponsored by the employer; or
- Revoke an existing election on a prospective basis, provided that the employee attests in writing that the employee is enrolled, or immediately will enroll, in other health coverage not sponsored by the employer.
As was the case in 2020, the employer can adopt all, some, or none of this relief. Employers can limit the number of election changes permitted and/or designate a time period during which such changes can be made, and the employer may limit the ability of employees to change from one type of health plan to another. Finally, the employee may not revoke an existing election for comprehensive health coverage by attesting to enrollment in a limited purpose dental and/or vision plan.
HRAs and FSAs
Pursuant to the CARES Act, employers were permitted to amend their plans to allow HRAs, health FSAs to reimburse expenses incurred for over-the-counter drugs without a prescription, as well as menstrual care products effective January 1, 2020. These expenses can also be reimbursed under HSAs and Archer MSAs. In the Notice, the IRS permits employers to amend their cafeteria plans (for purposes of the health FSA) and HRAs to reimburse these expenses effective January 1, 2020.
What Does This Mean For Employers
Pursuant to Notice 2021-15, employers must amend their plan to adopt any of these changes no later than the last day of the first calendar year beginning after the end of the plan year in which the amendment is effective. In other words, employers must amend a calendar year 2020 plan by December 31, 2021, and a calendar year 2021 plan by December 31, 2022. In the meantime, the employer must communicate these changes to employees and must operate the plan in accordance with the changes between the time the amendment is effective and when it is ultimately adopted by the employer. Employers should effectively communicate the changes to employees and ensure they operate in accordance with those communicated changes, including any limits they intend to impose.