The Internal Revenue Service (IRS) has released Rev. Proc. 2019-29, which contains the inflation adjusted amounts for 2020 used to determine whether employer-sponsored coverage is “affordable” for purposes of the Affordable Care Act’s (ACA) employer shared responsibility provisions and premium tax credit program. As shown in the table below, for plan years beginning in 2020, the affordability percentage for employer mandate purposes is indexed to 9.78%. Employer shared responsibility payments are also indexed.
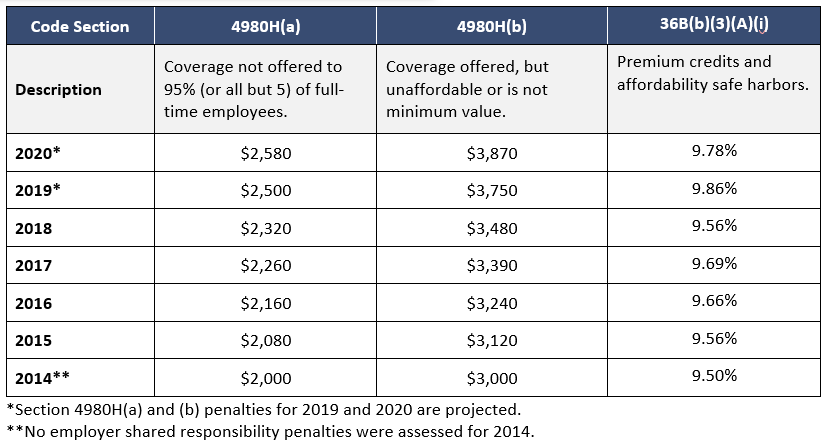
Under the ACA, applicable large employers (ALEs) must offer affordable health insurance coverage to full-time employees. If the ALE does not offer affordable coverage, it may be subject to an employer shared responsibility payment. An ALE is an employer that employed 50 or more full-time equivalent employees on average in the prior calendar year. Coverage is considered affordable if the employee’s required contribution for self-only coverage on the employer’s lowest-cost, minimum value plan does not exceed 9.78% of the employee’s household income in 2020 (prior years indexed above). An ALE may rely on one or more safe harbors in determining if coverage is affordable: W-2, Rate of Pay, and Federal Poverty Level.
If the employer’s coverage is not affordable under one of the safe harbors and a full-time employee is approved for a premium tax credit for Marketplace coverage, the employer may be exposed to an employer shared responsibility payment.
Note that as of January 1, 2019, the individual mandate penalty imposed on individual taxpayers for failure to have qualifying health coverage was reduced to $0 under the Tax Cuts and Jobs Act, effectively repealing the individual mandate. Although there is currently a lawsuit challenging the constitutionality of the ACA due to this change to the individual mandate penalty, the employer mandate has not been repealed and the IRS continues to enforce it through Letter 226J. The IRS has recently begun sending letters pertaining to calendar year 2017 reporting.
Next Steps for Employers
Applicable large employers should be aware of the updated affordability percentage for plan years beginning in 2020. Although the affordability percentage has not decreased significantly from 9.86% to 9.78%, employers should consider it along with all other relevant factors when determining contributions.
About the Author. This alert was prepared for Benefit Advisors Network by Stacy Barrow. Mr. Barrow is a nationally recognized expert on the Affordable Care Act. His firm, Marathas Barrow Weatherhead Lent LLP, is a premier employee benefits, executive compensation and employment law firm. He can be reached at sbarrow@marbarlaw.com.
This message is a service to our clients and friends. It is designed only to give general information on the developments actually covered. It is not intended to be a comprehensive summary of recent developments in the law, treat exhaustively the subjects covered, provide legal advice, or render a legal opinion.
Benefit Advisors Network and its members are not attorneys and are not responsible for any legal advice. To fully understand how this or any legal or compliance information affects your unique situation, you should check with a qualified attorney.
© Copyright 2019 Benefit Advisors Network. All rights reserved.